Urinary Tract Infection (UTI)
If you’ve ever experienced urinary tract infections (UTI), then you know how painful and frustrating they can be, especially if they keep coming back. There are, however, some simple measures you can take to prevent getting one in the first place and ultimately avoid the use of antibiotics.
Urinary tract infections are typically characterized by:
- frequent urination or a frequent urge to urinate
- lower abdominal or back discomfort
- burning pain during urination
- cloudy and foul-smelling urine
- painful urination (dysuria)
A UTI is the second most common type of bacterial infection diagnosed by healthcare professionals. The manifestations of a UTI depend on whether the infection involves the lower (bladder) or the upper (kidney) urinary tract and whether the infection is acute or chronic. Infections can range from asymptomatic bacteriuria to severe kidney infections which may cause kidney damage. Nevertheless, both should be considered as serious and addressed accordingly.
The urinary tract is constantly exposed to microorganisms that inhabit the gastrointestinal tract. However, the urinary tract generally resists infection through strong gut microorganisms and immunity. This resistance to infection is mainly ascribed to the versatility of the innate immune defences in the urinary tract. Recurrent UTI is an indication of limited healthy gut flora and an immune deficiency. This explains why it is difficult to cease a UTI with the use of antibiotics (reduce gut bacteria and immunity). It becomes a vicious cycle for many women, especially when there is also a hormonal influence.
A reduction of body defences creates a change in the body’s ability to resist infiltration from pathogens (viruses and bacteria). A decrease in the immune strength can eventually lead to:
- the washout phenomenon associated with voiding
- Interstitial cystitis
- defects in the protective mucus lining of the bladder
- other local immune deficiencies (immunity, elimination, pH)
- a shift in the vaginal microbiome
In an acute episode of cystitis (bladder infection) or a UTI, the symptoms disappear within 48 hours and are generally caused by the presence of Chlamydia trachomatis, Neisseria gonorrhoea, Escherichia coli (E. coli), Herpes simplex virus or vaginitis (Candida or Trichomonas).
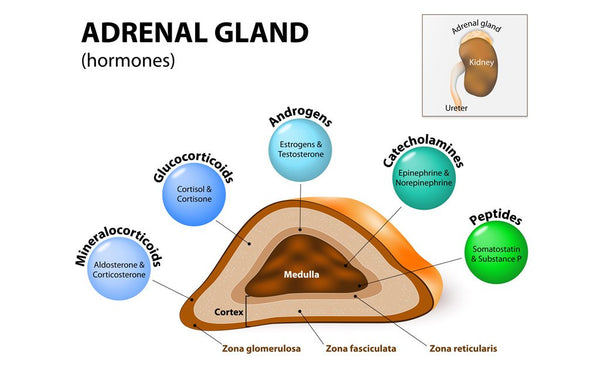
Hormonal changes during menopause may cause a UTI
Tissue thinning that occurs during menopause and the associated decline in oestrogen production affect not only the vaginal tissue but also the urinary tract. The lining of the urethra also becomes thinner and less elastic, increasing the likelihood of urinary tract infections and incontinence. Loss of bladder control especially when laughing, sneezing or coughing is quite a distressing problem many women face as they enter the menopausal phase.
Hormonal changes during the menstrual cycle and UTI
Some women are more likely to get an infection during certain times in their menstrual cycle, such as just before a period or during pregnancy. There is increasing evidence that fluctuations in the circulating levels of sex steroids (primarily oestrogen) can lead to functional changes in the female lower urinary tract. Many women will experience a UTI just prior or around the time of their menstrual period due to reducing levels of oestrogen at this time.
General recommendations to help prevent urinary tract infections
There are many triggers so avoiding as many as possible is important to prevent UTIs. Here are a few tips to lessen your chances of getting a urinary tract infection:
- “The solution to pollution is dilution.” Ensure that you are adequately hydrated as the body holds onto more metabolic toxins when fluid is insufficient. Lack of hydration also alters pH levels and causes opportunistic bacteria overgrowth.
- Drink herbal teas such as dandelion leaf, marshmallow root, and cranberry.
-
Avoid sugar as it encourages the proliferation of detrimental bacteria.
- Drink pure, unsweetened cranberry juice.
- Follow an alkalizing diet.
-
Reduce inflammatory foods in your diet.
-
Avoid foods containing yeast and treat any underlying Candida Infection, if present.
-
Supplement with a quality probiotic powder to encourage better resistance and promote healthy bacteria in the urinary tract. We also recommend drinking coconut kefir water every day.
- High doses of Vitamin C (1-2g every 2 hours) will have a local antibacterial effect. Choose a low-acid Vitamin C powder (calcium ascorbate combined with bioflavonoids) to avoid stomach upsets.
- Practice Kegel or Plyometric exercises to reinforce pelvic floor strength. You can perform Kegel exercises even while you are cooking dinner, driving or working at your desk! Just follow these easy steps:
- Contract the pubococcygeus (PC) muscle, the same muscle that you would use to stop urination mid-stream. Hold each contraction for 3 seconds, then relax for another 3 seconds between contractions. Repeat this contraction process 10 times.
- Now squeeze the PC muscle but this time release it as quickly as possible. Repeat this fluttering contraction 10 times.
- Repeat the entire sequence 3 times each day and increase the number of repetitions as you are able to.
- Drink plenty of water, and relieve yourself often. The simplest way to prevent a UTI is to flush bacteria out of the bladder and urinary tract before it can set in. If you’re well-hydrated, it will be tough to go too long without urinating.
- Wipe from front to back. Bacteria tend to hang around the anus. If you wipe from front to back especially after a bowel movement, they're less likely to make it to the urethra.
- Wash up before sex and urinate after it. Yes, you can get a UTI from having sex, especially if you're a woman. During sexual intercourse, thrusting can introduce bacteria up the urethra and into the bladder, increasing the risk of a UTI. Use soap and water before sex. This keeps bacteria away from the urethra. Urinating after sex pushes out any bacteria that may have entered the urinary tract.
- Steer clear of irritating feminine products. Skip douches, deodorant sprays, scented powders, and other potentially irritating feminine products.
- Rethink your birth control method. A diaphragm, spermicide, or spermicide-lubricated condom can make you more likely to get a UTI because they all can contribute to bacterial growth. If you often get UTIs and use one of these birth control methods, switch to a water-based lubricant for vaginal dryness and consider trying another birth control method to see if it helps.
Summary
An infection in any part of the urinary system – the kidneys, bladder or urethra – is referred to as a UTI and is more common in women. It usually occur in the bladder or urethra, but more serious infections can involve the kidney. Improving your diet, immunity, and gut health are imperative to reduce the severity and frequency of a UTI.
REFERENCES
Ronald A. The etiology of urinary tract infection: traditional and emerging pathogens. Am J Med. 2002;113(Suppl. 1A):14S–19S.
https://doi.org/10.1016/s0002-9343(02)01055-0
McCracken VJ, Lorenz RG. The gastrointestinal ecosystem: a precarious alliance among epithelium, immunity and microbiota. Cell Microbiol. 2001; 3:1-11
http://dx.doi.org/10.1046/j.1462-5822.2001.00090.x
Foxman et al. Urinary tract infection among women aged 40-65: behavioral and sexual risk factors. J Clin Epidemiol. 2001;54:710–718.
https://doi.org/10.1016/s0895-4356(00)00352-8